Research Spotlight:
Inflammatory Bowel Diseases
Inflammatory bowel disease (IBD) is the umbrella term for two digestive disorders: Crohn’s disease and ulcerative colitis (UC). Not to be confused with irritable bowel syndrome (IBS), IBD triggers an immune response, causing inflammation along the GI tract. The location and presentation of this inflammation distinguish Crohn’s and UC.
While there is no single cause for IBD, research suggests genetics, gut bacteria imbalance, and environmental factors may all play a role.
EPIDEMIOLOGY
Because IBD is often mistaken for IBS, viral infections, isolated peptic ulcers, and other gastrointestinal conditions, it’s difficult to determine the diseases’ prevalence. According to the CDC, healthcare administrative data estimates 2.4 to 2.8 million cases in the U.S., but national survey results suggest it might be as high as 3.1 million. Global rates are equally, if not more, challenging to measure. Despite this uncertainty, multiple studies suggest that IBD cases are rising.
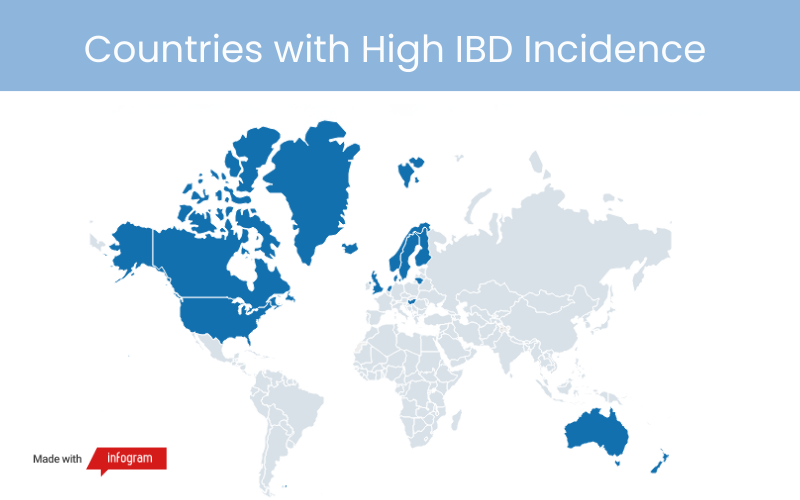
*Map based on findings published in The Lancet
WHERE FOOD COMES IN
IBD has the highest incidence rates in high-income countries, specifically the U.S., Canada, Northern Europe, and Australia, where processed foods comprise a significant portion of the average diet. Studies have found that as countries become more industrialized, whole-foods consumption decreases and processed foods consumption increases—as do IBD rates.
WOES OF THE WESTERN DIET
Unsurprisingly, inflammatory bowel disease has a long and complicated relationship with diet. Food may not be the singular cause or cure, but understanding its role in IBD onset, flare-ups, and baseline maintenance has the potential to reshape treatment and improve quality of life.
THE CONUNDRUM OF FIBER CONTENT
Because current research suggests a positive correlation between economic prosperity and IBD cases, it would be reasonable to assume that a whole-foods diet could be beneficial in reducing symptoms. Counterintuitive as it may be, the recommended protocol for IBD has historically been low fiber, with some studies linking this particular diet to a reduction in symptoms.
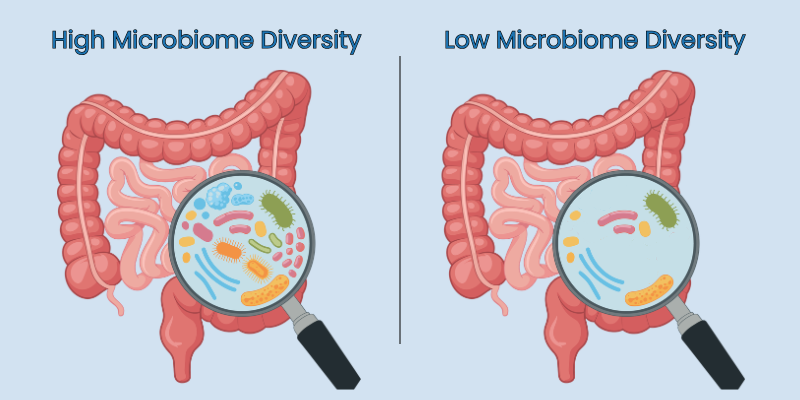
Nevertheless, many IBD specialists are skeptical of the standard dietary advice. Fiber-rich foods, ranging from vegetables, greens, and fruits to nuts, whole grains, and legumes, promote diversity in the gut microbiome, which has been positively linked to overall health. More research is needed to better understand the role of diet and the microbiome in IBD.
THE CURRENT TOOLBOX
Working with a dietitian is a crucial part of tailoring a diet to meet the needs of the individual. In addition to monitoring vitamin and nutrient levels, dietitians can help patients find eating habits that work for them. One strategy that was first developed to address IBS but has shown some promise among IBD patients is the low-FODMAP diet. Within this framework, fermentable, oligo-, di-, monosaccharides, and polyols are temporarily removed from a patient’s diet and then gradually reintroduced to spot trigger foods.
It’s important to note that the low-FODMAP diet is a short-term diagnostic tool best employed under the supervision of a dietitian; it is not a permanent diet. FODMAPs comprise many nutrient-rich whole foods that should not be eliminated en masse on a long-term basis. Furthermore, it has only been shown to manage IBS-like symptoms and does not necessarily address the inflammation at the root of IBD.
THE FLAWS OF FOOD DIARIES
Diet tracking is an important part of managing IBD symptoms and flare-ups. Healthcare providers can provide patients with resources to help them record the foods they’re eating, but ultimately the burden of responsibility falls on the individual. Not only do food diaries require a time investment, they are often incomplete, missing up to a fifth of foods consumed.
A NEW APPROACH?
FoodSeq, the technology driving Everyone EATS, can help fill the gaps of food diaries. Identifying plant and animal species via a stool sample offers an objective, more holistic view of an individual’s diet.
A Quick Note on Celiac Disease 🌾
Like Crohn’s and ulcerative colitis, celiac disease is a lifelong immune-related disorder marked by inflammation along the gastrointestinal tract, which can cause digestive distress and hinder nutrient absorption. But unlike IBD, celiac is directly tied to a specific protein, gluten, which is found in wheat, barley, and rye. Once gluten is eliminated, the gut should heal and symptoms should subside without any outside intervention.
While many foods, such as breads, baked goods, and beer, are well-recognized sources of gluten, the protein can also appear in less obvious places, including as a filler or stabilizing ingredient in processed foods. Although individuals can carefully choose certified gluten-free products, they may occasionally encounter unexpected gluten exposure through cross-contamination or hidden ingredients. By comparing Everyone EATS results with a food diary, it may be possible to identify potential sources of gluten that would otherwise be difficult to detect.
Further reading
IN THE NEWS
Diet and routine stool tests could help predict IBD flares, large study suggests” (Medical News Today)
“A new diet option for mild-to-moderate Crohn’s disease” (Sanford Medicine News Center)
“Two-Thirds Of Crohn's Disease Patients Benefit From Fasting Diet, Clinical Trial Shows” (U.S. News & World Report)
“New research charts sharp global rise in inflammatory bowel disease” (UChicago News)
“New Drugs, and Diets, Soothe Inflammatory Bowel Disease” (Scientific American)
“Can probiotics help calm inflammatory bowel disease?” (Harvard Health Publishing)
JOURNALS
“Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies” (The Lancet)
“Systems biology to unravel Western diet-associated triggers in inflammatory bowel disease” (Frontiers in Immunology)
“Microbiota in inflammatory bowel disease: mechanisms of disease and therapeutic opportunities” (Nature Reviews Microbiology)
“Food Processing and Risk of Inflammatory Bowel Disease: A Systematic Review and Meta-Analysis” (Clinical Gastroenterology and Hepatology)
“From west to east: dissecting the global shift in inflammatory bowel disease burden and projecting future scenarios” (BMC Public Health)
“The Gut Microbiota in Inflammatory Bowel Disease” (Frontiers in Cellular and Infection Microbiology)